Share this
How Should I Use My Health Savings Account (HSA)?
by Exchange Capital Management

It's that time of year again – open enrollment season for health insurance plans. Amid the maze of available plan options, there's a valuable tool that often gets overlooked: the Health Savings Account (HSA).
This often-untapped retirement planning tool packs three powerful punches in terms of tax benefits: a tax deduction when you contribute, tax-deferred growth inside the account, and tax-free withdrawals.
Unfortunately, most contributors use HSAs inefficiently and do not take full advantage of the benefits these accounts provide. Before diving into how you should use your HSA, let's start by getting to know what an HSA is and how it operates.
What is an HSA?
An HSA is a type of savings account that allows you to set aside money on a pre-tax basis to pay for current or future qualified medical expenses. It must be used in conjunction with a High Deductible Health Plan (HDHP). This type of health plan must satisfy certain IRS requirements regarding deductibles and out-of-pocket expenses. With an HDHP, you'll typically pay more upfront for medical costs before the plan starts covering services. However, in exchange, you often enjoy lower premiums compared to other medical plans.
The combination of a HSA and a HDHP can offer significant tax and savings advantages, potentially saving you money on health care, and giving you more control over how you allocate your medical dollars. Better yet, any leftover funds will roll over and stay in the account growing tax-free, with the option to invest in a wide array of investment options. Unlike the Flexible Savings Account (FSA), there is no “use it or lose it” provision. The account remains yours even if you change jobs, switch insurance providers, or retire.
Who is eligible?
To be eligible for contributions you must:
- Be covered under an HDHP as defined by the IRS. This can be purchased on your own or through your employer.
- Not have other, more comprehensive forms of coverage.
- Not be enrolled in Medicare.
- Not be listed as a dependent on another person’s tax return.
How much can be contributed?
Contributions can come from you, your employer, or anyone else, but there's a yearly contribution limit.
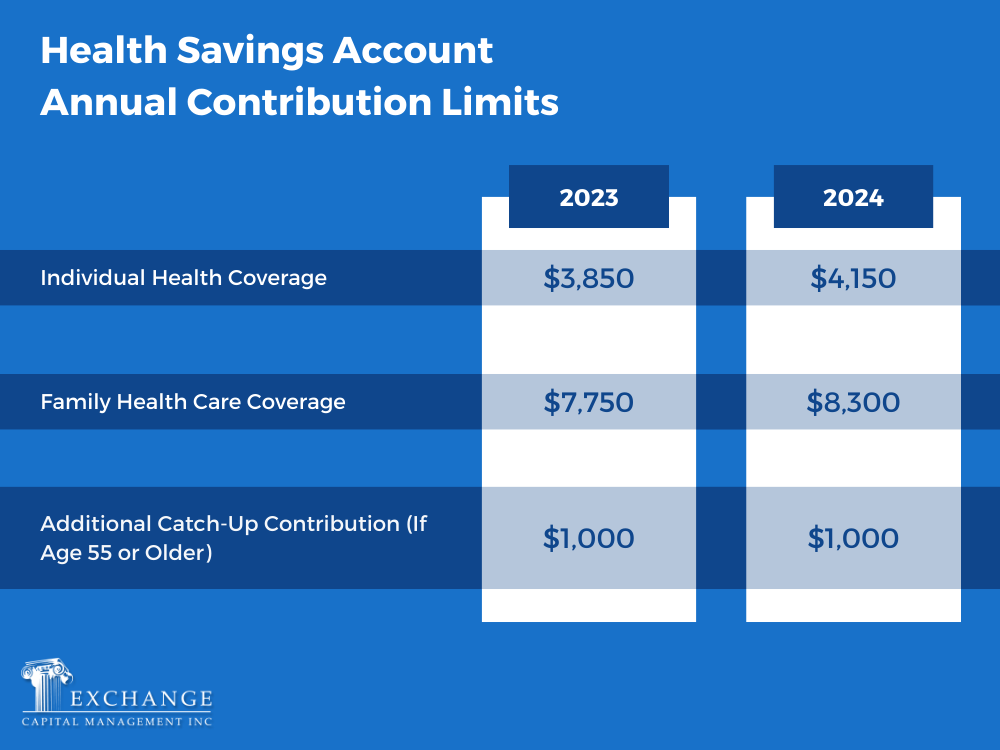
If your employer offers an HSA, your contributions are typically deducted from your paycheck on a pre-tax basis, similar to a 401(k). They might even sweeten the deal with their own contributions. If you have an HSA on your own, the tax break is still yours. These contributions are considered an “above the line” deduction on your tax return meaning you don't have to itemize them to claim your deduction. This could help you qualify for other deductions and credits. Also, unlike many other tax benefits, the HSA doesn't phase out at specific income levels, and it won't hinder you from saving in other retirement accounts.
How can HSA funds be used?
You can access your HSA tax-free and penalty-free to pay for qualified medical expenses at any time, including after you retire, stop making contributions, or become ineligible to contribute. The IRS determines the types of expenses that are qualified. They are listed in IRS Publication 502. The list is extensive and includes health plan deductibles and coinsurance, most medical, dental, vision, chiropractic services, and Medicare premiums (if age 65 or older).
Fortunately, you can use your HSA to cover your spouse's or dependents' medical expenses, even if they have their own non-HSA-eligible insurance. Plus, you can reimburse yourself for medical expenses from previous years, as long as they occurred after you opened your HSA. There’s no deadline for making withdrawals.
But here's the catch: if you dip into your HSA for non-qualified medical expenses, you'll owe regular income tax plus a 20% penalty. However, once you reach age 65 or become disabled, that penalty disappears. In this way, it's a bit like a traditional 401(k), but with the added perk of tax-free qualified medical expense withdrawals and no mandatory distributions kicking in at age 73.
What happens at the death of an HSA owner?
An HSA's tax treatment depends on who you designated to inherit the HSA. If it’s your spouse, the account becomes his or her HSA. If it passes to anyone other than your spouse, the account ceases to be an HSA and the 20 percent penalty no longer applies. However, the funds in the account become taxable income for the beneficiary or your estate. If you incurred qualifying medical expenses before death, the beneficiary or estate does not have to pay income taxes on the amount of those expenses as long as they are paid within a year of death.
What is the smart HSA strategy?
The tax benefits of an HSA make a powerful case for using one. However, according to a recent report by Devenir Research, most people under-utilize these accounts. Only 32 percent of HSA assets are held in accounts where they can be invested for growth. Instead, 68 percent of assets are held in HSA bank accounts which pay little to no interest. Using this strategy, you will lose out on the opportunity for tax-deferred growth and potentially larger tax-free distributions in retirement.
To gain the most benefit from an HSA, we should rethink how we view and use these accounts. Instead of seeing your HSA as a go-to fund for immediate medical needs, you should view it as an additional form of retirement savings. It’s often recommended to invest in the account as early as possible and avoid tapping into it until retirement. For this strategy to be effective, you'll need to have the financial means to not only contribute to the account, but also have additional funds to cover healthcare costs in the meantime.
What is the potential burden of healthcare expenses in retirement? According to the Fidelity Retiree Healthcare Cost Estimate, a 65-year-old couple can expect to spend $315,000 in healthcare throughout their retirement. Obviously, saving for health care should be an important part of retirement planning.
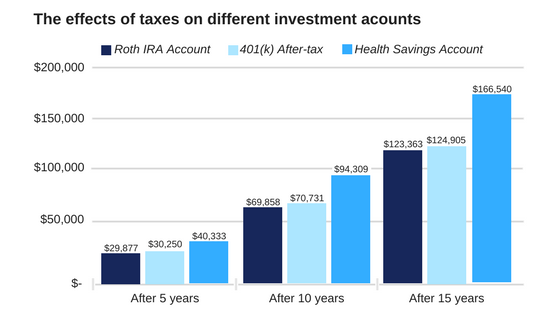
The above chart illustrates how saving in an HSA can accumulate over time. It assumes $5,000 (post-tax) in annual contributions to a Roth IRA, a $6,750 (pre-tax) annual contribution to a 401(k) with a 25% tax on distributions, and a $6,750 (pre-tax) annual contribution to an HSA with no tax on distributions for qualified health care costs. Each account assumes an annual growth rate of 6%. After 15 years the amount available for health care costs from the HSA is 33% larger than the 401(k) and 35% larger than the Roth IRA due to its triple tax advantage.
The Bottom Line
If you're reviewing your insurance benefits this open enrollment season, consider the benefits an HSA provides. Additionally, if you're eligible for an HSA, or have one already, ask yourself if you're taking full advantage of the opportunity. Thinking about future medical care costs isn't fun but preparing ahead of time makes any challenge more manageable.